Ehlers-Danlos Syndrome, Classic and Classic-like
The Ehlers-Danlos syndromes (EDS) are a group of 13 related conditions that affect connective tissue (1). Connective tissue is found everywhere in the body. It connects other types of tissues, separates them, and supports them. Examples of connective tissue include bone, cartilage, fat, blood, and lymphatic tissue. When connective tissue is abnormal because of a disease, a variety of problems result.
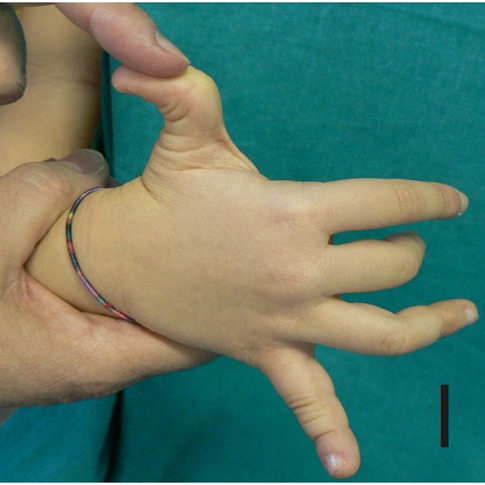
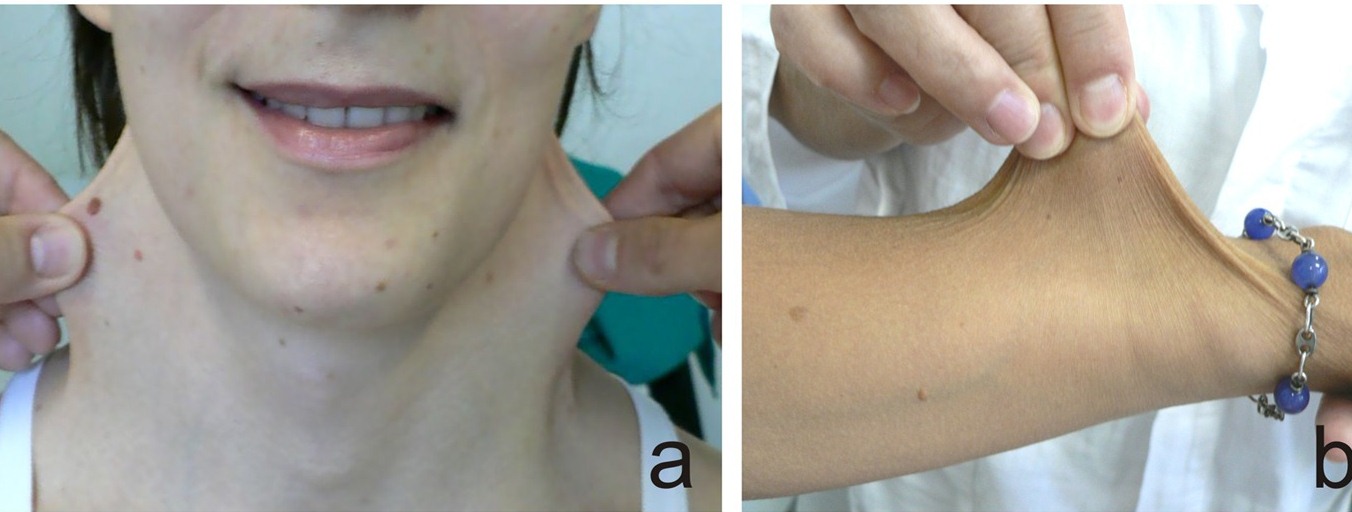
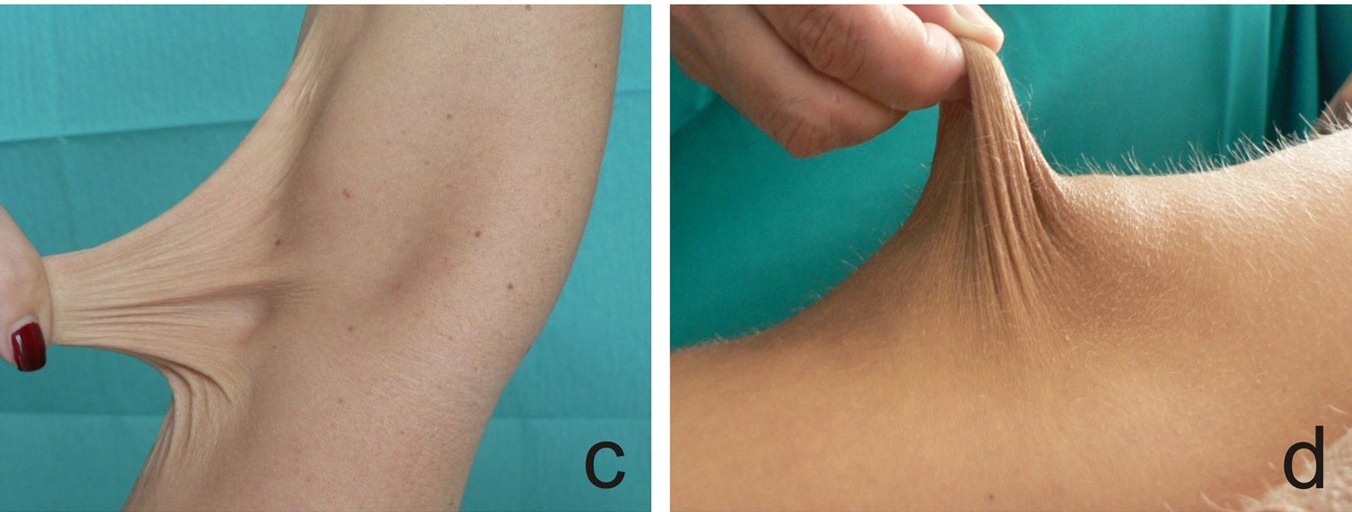
For example, certain problems happen in all of forms of EDS. The first is joint hypermobility (often called loose or double joints). People with EDS can often move their joints in ways that are impossible for most unaffected people. The photograph at the bottom of this page has an example (note that many people without EDS have loose joints, so having joint hypermobility does not mean that you have EDS). The second thing that happens in every type of EDS is stretchy (hyperextensible) skin. This feature is nearly universal in some types of EDS (such as type 1, the classical form). In our literature survey, we found that stretchy skin occured in less than half of people with the hypermobile and vascular forms, more than half of patients with the periodontitis type, and in a large majority of people with the arthrochalasia type (>80%).
Many forms of EDS happen because of mutations in genes that make collagen, which can be thought of as both holding the body together and strengthening it. Collagen gives structure to muscles, tendons, skin and bones. In most people, it is abundant in these tissues. In people with EDS, collagen may not be as strong as it should be, or there may not be enough of it. For example, skin and joints may be loose because they don't have enough collagen to hold them together securely, or because the collagen they have is weaker than it should be.
Doctors and other medical professionals assess joint hypermobility with a scoring system called the Beighton score, which was developed in the early 1970s (2). This simple system scores your ability to move a joint past certain angles. The highest score is 9 points, and higher scores mean greater joint hypermobility. Generally speaking, scores of 4 or higher (at any time, past or present) indicate joint hypermobility. Many EDS patients have scores of 8 or 9, although many have lower scores, and a minority do not have hypermobile joints. Interested readers may wish to see a basic description of the scale with a video and photos or a more technical description.
Joint hypermobility puts EDS patients at high risk for joint dislocations and partial dislocations (called subluxations). These problems can be painful, and in some cases, debilitating. Surgical procedures have been used to improve skeletal stability and improve quality of life; for examples and reviews, see references 3-5. However, experts tend to agree that non-surgical options should always be exhausted first, and careful discussions with doctors are important in this decision.
Tissue fragility is another common feature of EDS. This problem is very serious in the vascular type of EDS (vEDS). The type of collagen affected in vEDS plays a role in supporting blood vessels. When the integrity of their support system is affected, blood vessels can rupture spontaneously. This problem is especially dangerous because it affects medium and large blood vessels, as well as small ones. It also affects the bowel. Surgery on a person with vEDS must be performed with great care in order to avoid serious complications. This problem may also happen in kyphoscoliotic EDS (kEDS), but it is less common than in vEDS. Alternatively, while people with the hypermobile form (hEDS) are also prone to blood vessel ruptures, ruptures tend to occur in the small blood vessels. Tissue fragility can also lead to hernias and problems in pregnancy. Fragile skin is also a common manifestation of EDS, especially in people with the classic, kyphoscoliotic, and periodontitis types.
Tissue fragility in EDS can also lead to hernias and problems in pregnancy. Fragile skin is also a common manifestation of EDS, especially in people with the classic, kyphoscoliotic, and periodontitis types.
A new classification system for EDS was released in 2017 (1). It's called the 2017 International Classfication for the Ehlers-Danlos Syndromes. This new system names 13 different subtypes of EDS. It relies primarily on descriptive terms for different types of EDS (e.g. vascular EDS, meaning that it affects blood vessels prominently). Two other systems existed before this one. They were named Villefanche [1998] and Berlin [1988]. Both systems used names and numbers. The numbers in the new system are different from the old ones, and we've included the old ones here. Advances in genetics have allowed to researchers to find genes that cause different subtypes of EDS, which has allowed them to separate the old classic subtype (numbered 1 & 2) of EDS into 2 different subtypes.
- 1. Classical EDS (cEDS; formerly type 1/2)
- 2. Classical-like EDS (cEDS; formerly type 1/2)
- 3. Cardiac-valvular (cvEDS)
- 4. Vascular (vEDS)
- 5. Hypermobile (hEDS; formerly type 3)
- 6. Arthrochalasia (aEDS; formerly type 7a/b)
- 7. Dermatosparaxis (dEDS; formerly type 7c)
- 8. Kyphoscoliotic (kEDS; formerly type 6)
- 9. Brittle Cornea syndrome (BCS)
- 10. Spondylodysplastic (spEDS)
- 11. Musculocontractural (mcEDS)1
- 12. Myopathic (mEDS); type 12
- 13. Periodontal (pEDS; formerly type 8)
EDS affects women more commonly than men. In the literature survey we did for our analytics tool, we counted the number of male and female patients while we were characterizing in six different types of EDS. Altogether, we analyzed data from ~1,200 patients. Sex information was available for ~1,100. The table below shows that although more EDS patients are women in each type of EDS, the female:male ratio varied between each type. For example, females dominated the individuals reported with the hypermobility type, while males comprised a substantial minority of kyphoscoliotic and arthrochalasia patients. The distribution was roughly even in the periodontal type. However, the low number of case reports for these three types of EDS may have affected the outcome of this small analysis.

Above: Percentages of male and female patients with different types of EDS. Source: FDRF via published literature.
According to NIH's Genetics Home Reference (see link at right), the prevalence of all forms of EDS is roughly 1 in 5,000 worldwide. The Gene Review article linked to at the right estimates that type 1 of EDS occurs in one birth per 20,000; figures for clEDS are not known, nor is there a Gene Review article for clEDS.
Clinical information
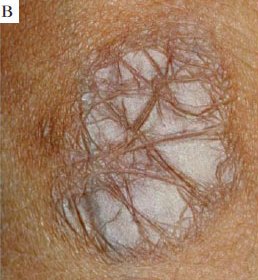
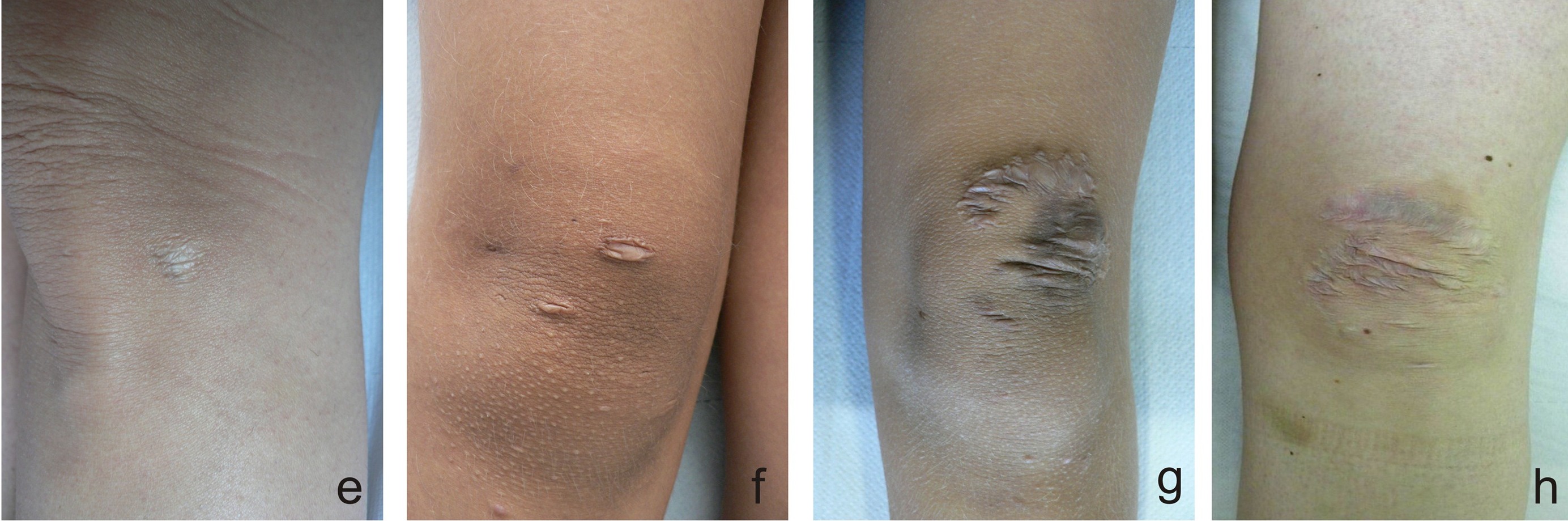
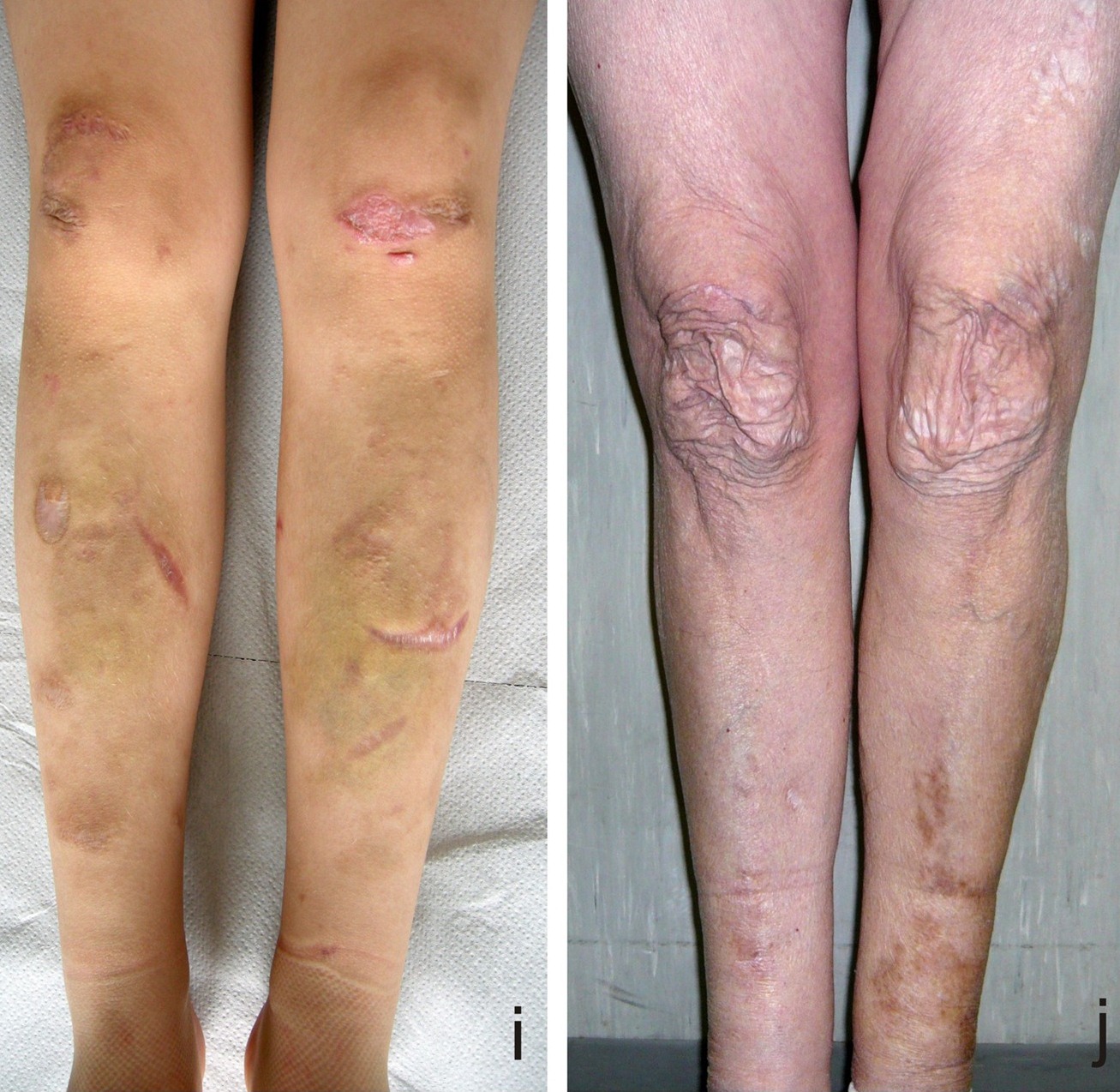
cEDS is a common forms of EDS (another is the hypermobile form). These two conditions are very similar, but are caused by mutations in different genes. Their most striking features are joint hypermobility and loose skin that bruises or tears easily, and heals slowly. The skin over healed wounds may also stretch with time, creating scars that are wide and odd-looking. See photos on this page for examples of skin problems in cEDS and clEDS. Like EDS in general, cEDS and clEDS are more common in women (in our survey of ~300 published cases of classic EDS, 64% of patients were female).
The clinical features of cEDS and clEDS tend to overlap with other forms of EDS, although there are differences that help distinguish them from the other forms (see Differential Diagnosis, below). In general, the following features occur commonly in cEDS and clEDS:
- Loose or stretchy skin
- Joint hypermobility
- Joint dislocations or subluxations
- Joint and/or muscle pain and/or headaches
- Smooth, velvety skin
- Fragile skin that may scar abnormally
- Slow wound healing
- Easy bruising (bruising may even occur spontaneously)
- Molluscoid pseudotumors or subcutaneous spheroids (see photos and discussion below)
- Flat feet
- Weakness
- Fatigue or easy loss of energy
- Cardiac problems in a minority of patients, including mitral valve problems and aortic root dilatation
- Flat feet
Signs and symptoms of classical and classical-like EDS
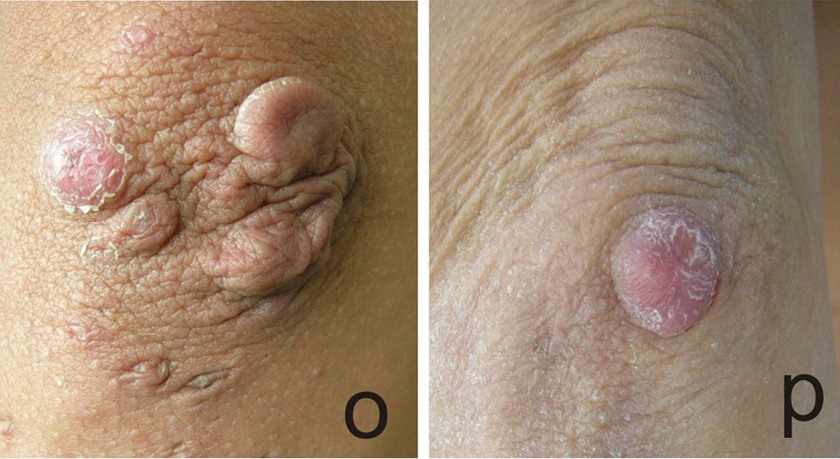
Molluscoid pseudotumors (see photos below) are fleshy calcified lesions that form over scars at pressure points on the body (often the elbows and knees). Alternatively, subcutaneous spheroids are small calcified nodules that form under the skin. They can be felt through the skin and may be moved. They form from fat globules that lose their blood supply and become calcified. They are visible on x-rays or scans.
Diagnosis and Testing
Classical EDS is an autosomal dominant disorder. This term means that it is usually passed from one affected parent to a child. However, it can also occur sporadically in a person without an affected parent. Each form appears to occur relatively half the time.
Mutations in the genes are COL5A1 and COL5A2 are associated with cEDS. More than 90% of cEDS patients have a mutation in one of these genes (1,6). The remaining cases are caused by mutations in COL1A1; COL1A1-EDS may be more severe than EDS caused by the COL5A1 and 2 genes. Mutations in COL1A1 are associated with a number of other medical conditions, including the arthrochalasia type of EDS, osteogenesis imperfecta, and Caffey disease. A few cases that resembled cEDS may be caused by mutations in COL1A2 (1).
The criteria below were established as part of the 2017 classification system (1). For a diagnosis, a patient must have the first major criterion (skin hyperextensibility and atrophic scarring) AND the second major criterion OR three of the minor criteria. Identification of a mutation is also essential.
Major criteria
- Skin hyperextensibility and atrophic scarring (see photos)
- Generalized joint hypermobility
Minor criteria
- Easy bruising
- Soft, velvety, doughy skin
- Fragile skin
- Molluscoid pseudotumors
- Subcutaneous spheroids
- Hernia (past or present)
- Complications of joint hypermobility (sprains, luxations/subluxations, pain, flexible flat feet
- A parent, sibling, or child who meets these criteria
Classical-like EDS is an autosomal recessive disorder. This term means that a mutated copy of the gene must be inherited from each parent. In the past, clEDS was grouped together cEDS as Classic EDS (types 1/2), but recent advances have allowed it to now be classified as a standalone subtype of EDS. It is caused by mutations in the gene TNXB.
The criteria below were established as part of the 2017 classification system (1). For a diagnosis, a patient must have all three major criteria and a family history compatible with autosomal recessive transmission. Identification of a mutation is also essential.
Major criteria
- Skin hyperextensibility with velvety skin and NO atrophic scarring
- Generalized joint hypermobility with or without dislocations (when they occur, they are most frequently at the shoulder and the ankle).
- Easy bruising (bruises may even appear spontaneously)
Minor criteria
- Foot deformities: broad/plump forefoot, short fingers (brachydactyly) with excessive skin; flat feet (pes planus); bunions (hallux valgus); piezogenic papules
- Swollen legs (common in heart failure patients; in its absence in EDS)
- Mild muscle weakness
- Axonal polyneuropathy
- Atrophy of muscles in hands and feet
- Prematurely aged (acrogeric) hands, mallet finger(s), bent fingers (clinodactyly), short fingers (brachydactyly)
- Sagging (prolapse) of the vagina or uterus
It is important to remember that there is a lot of overlap between the different forms of EDS. This fact means that, in the absence of laboratory testing, accurate subcategorization of EDS in a patient may be difficult or even impossible.
Differential Diagnosis
Other forms of EDS. The differential diagnosis for cEDS and clEDS includes all the other types of EDS. All forms of EDS involve joint hypermobility, and most also feature very soft, lax skin, as well as a variety of internal problems that result from weak or loose connective tissue (e.g. hernias, spinal column deformities, flat feet). However, some forms of EDS are more severe than others.
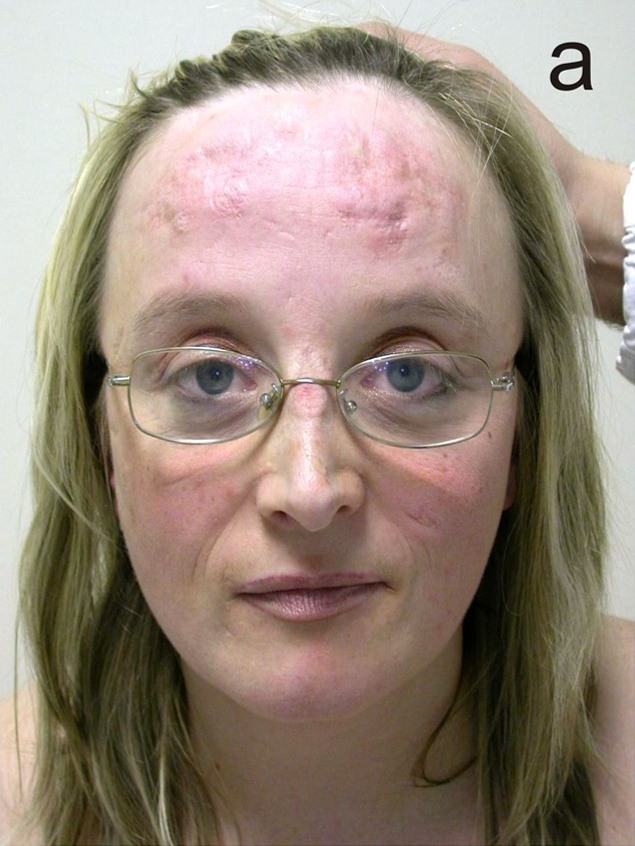
cEDS and clEDS may be distinguished from the rarer vascular and kyphoscoliotic types by genetic testing: the vascular form is caused by mutations in COL3A1, and the kyphoscoliotic form is caused by mutations in PLOD1 or FKBP14. In addition, these conditions are generally (although not always) much more severe than the classic form. Patients with vascular EDS have a particular facial phenotype that is not shared by classic type patients,, and those with the kyphoscoliotic form tend to have severe spinal deformities. Note also that EDS-vascular patients are prone to spontaneous ruptures of large blood vessels that may be fatal. For this reason, clinicians may wish to use genetic testing to definitively rule out this form of EDS in any patient suspected of having EDS.
The hypermobile form of EDS (hEDS) is a relatively mild form of EDS. As its name implies, joint hypermobility is the primary feature of this form of EDS. The skin in hEDS patients is typically not as stretchy as it is in patients with the classic form, although exceptions apply. In addition, hEDS patients are prone to hearing loss, which does not appear to be a feature generally associated with cEDS and clEDS. Atrophic scars also do not appear to be a general feature of the hypermobile form of hEDS.
Overall, joint hypermobility occurs in a variety of medical conditions, and many people without a medical condition have lax joints. In fact, when not part of a disorder, hypermobile joints confer an advantage in sports such as gymnastics and ice skating, as well as in certain forms of dance.
Marfan syndrome. Most medical conditions involvong lax joints are relatively easy to distinguish from EDS, but some are not. Marfan syndrome is an example. Like EDS, Marfan syndrome is a connective tissue disorder and patients have lax joints. Marfan patients generally have a body type called a Marfanoid body habitus. This term means that a person is tall and slender, with long arms, hands, fingers, legs, feet and toes. A Marfanoid body habitus occurs in a minority of EDS-H patients, but it does not appear to be generally associated with classic EDS. The Marfan Foundation has many photographs of Marfan patients of different ethnicities. Unlike EDS patients, Marfan patients do not appear to have fragile skin and blood vessels.
Williams syndrome. The Gene Review on classic EDS (see link at right) has a list of other conditions that are part of the differential diagnosis for EDS. They include , which may be distinguished from classic EDS by specific intellectual disabilities, a specific personality type, and other factors. The list of conditions also includes Loeys-Dietz syndrome, Stickler syndrome, and a number of other conditions.
Cutis laxa. Superficially, the stretchy skin found in most forms of EDS may be confused with cutis laxa type 1 and type 2, as stretchy skin is also a feature of these conditions. However, the skin in cutis laxa patients tends to sag and does not return to its normal position after being extended. Cutis Laxa patients often have a prematurely aged appearance.
References
- 1. Malfait F et al. (2017) The 2017 International Classification of the Ehlers-Danlos Syndromes Am J Med Genet C 175(1):8-26. Abstract on PubMed.
- 2. Beighton P et al. (1973) Articular mobility in an African population. Ann Rheum Dis 32(5):413-418. Full text on PubMed.
- 3. Cole AS et al. (2000) Recurrent instability of the elbow in the Ehlers-Danlos syndrome. A report of three cases and a new technique of surgical stabilisation. J Bone Joint Surg Br 82(5):702-704. Full text from publisher.
- 4. Weinberg J et al. (1999) Joint surgery in Ehlers-Danlos patients: results of a survey. Am J Orthop 28(7):406-409. Abstract on PubMed.
- 5. Shirley ED et al. (2012) Ehlers-Danlos syndrome in orthopaedics. Etiology, diagnosis, and treatment implications. Sports Health 4(5):394-403. Full text on PubMed.
- 6. Ritelli M et al. (2013) Clinical and molecular characterization of 40 patients with classic Ehlers-Danlos syndrome: identification of 18 COL5A1 and 2 COL5A2 novel mutations. Orphanet J Rare Dis 8:58. doi: 10.1186/1750-1172-8-58. Full text on PubMed.
- 7. Beighton P et al. (1969) Variants of the Ehlers-Danlos syndrome. Clinical, biochemical, haematological, and chromosomal features of 100 patients. Ann Rheum Dis 28(3):228-245. Full text on PubMed.
- 8. Bicca EB et al. (2011) Classical Ehlers-Danlos syndrome: clinical, Histological and ultrastructural aspects. An Bras Dermatol 86(4 Suppl 1):S164-167. Full text from Scielo.